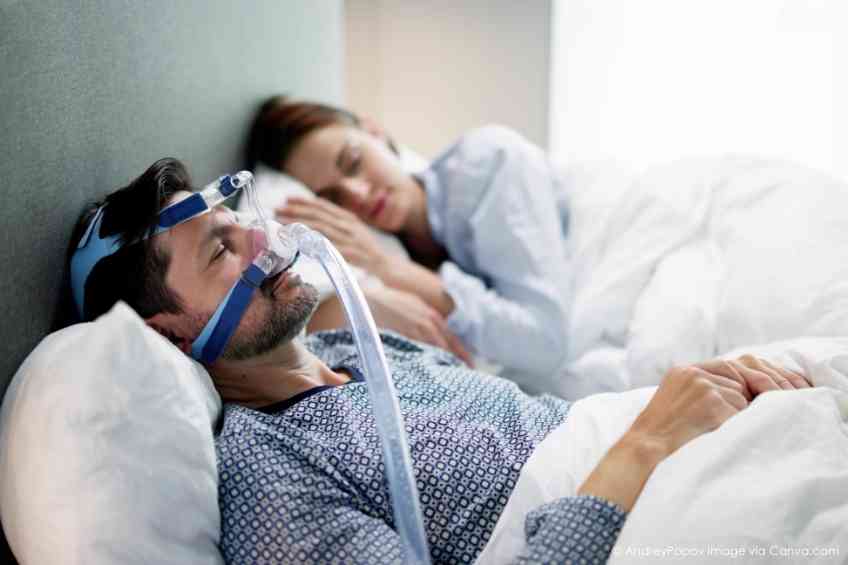
Lots of people suffer from lousy sleep. For a growing number of individuals, the problems go deeper as they face the realization that they are experiencing sleep apnea in one form or another. In fact, approximately one billion people suffer worldwide from this problem, of which about 40 million are in the U.S. Ultimately, the problem comes down to an individual’s air passage getting blocked for at least 10 seconds at a time, reducing their oxygen intake levels and disturbing their sleep patterns. Lots of times snoring is involved. Yet despite the growing awareness of sleep apnea’s impact, there are still a lot of unknowns for sufferers. Thanks to sleep apnea expert Dr. Andrew Namen who spoke to WellWell recently about the causes, symptoms, threats and treatments. He pointed out that the problem is nothing to sleep on.
Exactly what is sleep apnea? Is it an umbrella phrase for many disorders or problems?
There are a number of different sleep apnea syndromes out there. There are two major categories, obstructive and central. The most common thing that we see is obstructive apnea, where patients are making an effort to breathe but, there’s either reduced airflow or they stop breathing altogether while they’re sleeping. And when that happens, we’re looking at a drop in their oxygen level that occurs and a reduction in flow for at least 10 seconds to qualify for that diagnosis. Now, central sleep apnea is a little different where you’re not making any effort. No flow or reduced flow, and again 10 seconds with an appreciable drop in oxygen levels. Those two disease states differ based on the causality of those two diseases. Obstructive sleep apnea is what we commonly see among people who are gaining weight or heavier or have craniofacial disease. Central sleep apnea tends to be one that’s related to other medical conditions like strokes or heart disease. And some patients are neither one nor the other but can have features of both.
Is sleep apnea always focused on the inability to breathe or the cutting off of oxygen? How many people are affected by this?
It has been estimated to be as many as a billion people worldwide. It’s approximately 25 percent of the population in the United States. And rates of this disorder are increasing for a couple of reasons. One is the overall body mass index has increased among patients across the United States. Also, people are living longer and when you have more conditions or medical problems, sleep apnea also tends to be more prevalent with the more problems that you have. It’s one of those things that happens because we’re living longer with diseases as well as our bodies are changing and we’re getting heavier as a country and as a world.
Does the environment play a factor in this?
In some instances, and not the most common, our environment can affect our breathing. And so, people with respiratory disorders that tend to be sensitive to their environment may demonstrate more breathing-related sleep disorders like sleep apnea, making it more challenging for those folks. For instance, patients with asthma may be very sensitive to their environmental triggers. If they have sleep apnea as an underlying condition they didn’t know about and then they start having asthma issues, they may notice more apnea-like symptoms making the condition worse. It also can make the condition more obvious. Maybe they didn’t know they had it and family members recognized it when they were sleeping.
What other risks occur from sleep apnea that raise the risk for other diseases?
There are a number of different risk factors with it. We mentioned weight. For adults mainly, some have what’s called craniofacial changes. So even though it’s part of their normal anatomy, they were born with it. Parents bequeathed it to people who may have a recessed jaw, tight nostrils or a narrow airway. All those things are looked at by physicians to say you’re a person who’s at risk for breathing-related sleep disorders or sleep disorder breathing. The other conditions that can make it worse and cause more sleep apnea are heart failure patients, patients who suffer strokes if it affects their airway collapsibility, people with neuromuscular disorders can have more apnea-like episodes, folks who have other common breathing disorders and patients who are diabetics – people that tend to be heavier and have issues with sugar.
What are the risks of sleep apnea? Is it just that you’re going to have a lousy night’s sleep or is it more serious?
Sleep apnea does cause a lot of insufficient sleep where you have what’s called micro arousals that lead to an unrefreshed night. But sleep apnea alone has been attributed to high blood pressure. New onset rhythm disturbance like Atrial FIB is one of those conditions and challenges with augmenting other conditions, even though it’s more associated with heart failure. It can make heart failure worse.
Why do we talk about it more now? Why is there greater awareness?
Our science has gotten better. We have learned more about sleep apnea and its potential impact. Sleep apnea is one of those conditions that have been difficult to recognize even for medical sciences. Understanding its impact is more long-term, so somewhat more difficult to understand its impact on a person’s health condition, except with very well-designed long-term studies that kind of say ohh we see that signal creating that problem. And so those have made it challenging for us to understand the impact of sleep apnea. The second thing is we’re just getting heavier as a country and as a world, and because of increasing weights, we’ve seen a higher increase in sleep apnea rates. We are also living longer with comorbid conditions that are affected by sleep apnea. So what we also recognize is that sleep apnea has been associated with folks coming to the hospital and in some cases, you’re maybe going to go through an elective procedure and your doctor and the anesthesiologist ask you, hey do you have these problems that we attribute to sleep apnea and so trying to minimize or mitigate those events in the hospital, whether your oxygen drops, getting more pneumonias or having a respiratory event may be avoided if identified and detected.
Most people are going to think that if you’re snoring, you have sleep apnea. Is it an absolute link?
No, not at all. There are a lot of people who have just simple snoring disorders without any associated gasping. And I would say a lot of folks are like that.
What are some of the other symptoms and what are the potential treatments?
I will say, that patients sometimes have a hard time identifying their symptoms when they sleep at night because we’re in that deep phase. Often we recognize the problems of sleep apnea from the bed partners raising the concern of stopped breathing. One major symptom is that they choke at night. Another major symptom is they’re waking up all the time and very restless and it appears to be related to their breathing and snoring where they just stop breathing. So those symptoms are seen in sleep apnea but are not the only symptoms that are seen. Sometimes snoring is the only symptom that they may have at night and it could be related to sleep apnea, but it might also be some of the other symptoms we see during the day. Feeling tired all the time, even despite a good night’s rest. Having difficulty with focus and memory. Having some snoring with some focus issues or memory loss that you can’t attribute to anything else or feeling unrefreshed after a restful night’s sleep and feeling sleepy during the day where you want to take naps when everybody else doesn’t want to and you’re not accustomed to doing it. Falling asleep during passive activities like sitting in the car for an hour as a passenger or talking to someone during conversation or just relaxing in a park feeling the pressure of sleep or dozing during that time.
You can judge whether you are having a lousy night’s sleep, but it must be difficult to judge whether you have these other symptoms.
It is difficult for them to judge and I often have patients who don’t quite believe their bed partner. So, I think our bodies have learned to accommodate challenges to our respiratory system and to our sleep. And because of that, the person with sleep apnea oftentimes cannot believe what their bed partner is witnessing because they’ve lived with it for so long. And those are some of the other challenges. I mean, if you think a stop-breathing episode lasting 10 seconds with the drop in your oxygen level and you’re not waking up fully to it: you’re having what we call these micro-arousals. Well, what we used to do is measure patients’ blood pressure during these episodes. And very simply, the more severe the apnea, the higher the blood pressure in some cases. Even reaching very high pressures and that’s why it has been attributed to high blood pressure control, strokes and heart attacks.
What is the relationship to memory in sleep apnea?
There’s been quite a bit of studies looking at cognition and sleep apnea. And I would say the impact is twofold. One, the number of sleep apnea events and unrefreshed sleep. And this is only a part of the equation. The second is drops in oxygen levels, so if you’re having drops in your oxygen level and arousals and stop breathing episodes and inflammatory mechanisms that start occurring because of these events, it can affect your neurotransmission. It can affect some of what we call white matter changes in the brain. Some of these things have been well described in the literature, but still, we’re trying to understand it and identify mechanisms to mitigate those effects.
How do we identify it once we go to a professional? Is there a simple test?
Once your professional has identified that you have symptoms that are consistent with the possibility of sleep apnea, those are the folks who should be tested. And, there are a number of great new devices making it very easy for patients to be tested, especially patients who are relatively healthy and don’t have a lot of medical conditions. It’s called a home sleep test and they come in a lot of different versions. They have improved their accuracy in identifying patients with sleep apnea as well as helping provide access for patients to get a sleep study, whereas before it was always inside a lab. So now we can do studies at home called home sleep testing.
Do they have to be prescribed by a doctor or medical professional?
Yes, they do. Now you have consumer technology that’s out there that helps you try to understand if a person is at risk. Now, not all of those are well-controlled or FDA-approved for this stated indication. So, we always ask folks to go to the American Academy of Sleep Medicine website and take a look at consumer technology. We provide some great insight into that arena. At the same time, the home sleep test that is FDA-approved and cleared by the American Academy of Sleep Medicine (AASM) has been helpful in accurately identifying patients with sleep apnea. Now, if you’re a person who has a significant medical condition, severe COPD or heart failure or a history of stroke or rhythm disturbance, your doctor may feel like you’re more appropriate for an in-lab test because it is our gold standard. It is our best test for identifying sleep apnea. You should do the right test when you’re the right patient for that test and avoid the simple test just because you’re a little overwhelmed by the in-lab test. We want to identify the patient that really needs to be studied.
So, we’ve identified if somebody has sleep apnea, what do we do next?
It depends upon the sleep apnea, the severity of the sleep apnea and that conversation with your provider. So, you know for the patients with medical conditions that are symptomatic, a trial of positive airway pressure, what is commonly referred to as CPAP, where you get a constant flow of air may be needed. If you think of the airway being like a doughnut and collapsing during sleep apnea obstructive events, that positive airway pressure keeps that airway open and in a better size, then apneas don’t occur. It takes pressure to kind of inch that airway open. That being stated, there are a number of different positive airway devices out there. There are different ways we deliver that positive airway pressure, all to optimize the patient’s interface with something foreign to them but all for the benefit of reducing those events (the snoring, the choking, the gasping) hopefully relating to improvement in their blood pressure or blood sugars and other clinical conditions.
Can sleep apnea be cured or reversed? Is someone always going to have to use a device?
I’ve done this for a couple of decades and I’ve had patients who have been on it before they met me and are still on it today. So that being said, yes, in some cases, people do live their entire lives with CPAP. And are very happy that they do. I also have patients who have been challenged by CPAP and have sought alternative therapies which can also include, especially in those folks that have mild to moderate disease, something called an oral appliance, which is something a sleep dentist or a dentist that practices in sleep can provide to help keep the jaw from collapsing where air and your tongue advance. And then other therapeutics are out there that are intended to keep the tongue out of the way of obstruction and the back of the airway open. Something now called the hypoglossal nerve stimuli has also been demonstrated to reduce the number of apnea events as well as hopefully improve the long-term outcomes of these patients.
For those who have exacerbated their sleep apnea because they’ve gained weight, would losing weight relieve or mitigate sleep apnea?
There are a lot of folks who see their sleep apnea improve. Some people see a surgeon for their sleep apnea, which in some smaller cases improves. We also like to help our patients have improved sleep hygiene, which means making sure their sleep environments are nice and cool, no distractors, no bright lights and no telephone close to the bedside. And we also like them to have a better sleep apnea life. This means early morning exercise routines and trying to lose that weight that kind of may have been the cause of pushing them there. But although we attribute it to weight, weight alone is not the only cause of sleep apnea, and I don’t want it to be assumed that it only occurs in heavier patients. It does not. About 20 percent of patients have a normal BMI. So, for the heavy patient, optimize your weight and lose weight that has been associated with a reduction in at least the severity of sleep apnea and, in some cases, a resolution of their sleep apnea.
What is the percentage of people who cure or eliminate their sleep apnea?
In some estimates with adequate weight loss, up to 10 percent of patients may have improvement or near complete resolution of their state.
What do you want people to do or take away from this conversation?
I think having that conversation with their provider, especially if they have symptoms. Don’t be afraid of it. For those who don’t want to go through the expense or see a doctor regarding it, I tell them you will save far more money understanding your disease state. Many studies have shown that it’s more cost-effective for a patient’s health to be identified and to treat that problem before seeing a specialist. Let’s say what we want you to do is explore the symptoms. Hopefully, this podcast will help you identify some of those symptoms that have led to that discovery. Recognize that having a sleep study is very easy now and that it’s accessible. It’s not as expensive and if it helps you identify the problem, you can then go on to the road of recovery. And not all treatment is CPAP. There are a number of other therapeutics, although CPAP is the standard of care for symptomatic sleep apnea with moderate to severe disease. Still, it is not for everybody. Patients can receive other therapeutics like oral appliances. So don’t be afraid of the treatment either. Have that conversation, explore the symptoms, be tested and try to achieve a better, healthier sleep apnea lifestyle.

About Andrew Namen, MD, FCCP, FAASM
Dr. Andrew Namen is a sleep apnea expert and a pulmonologist with Wake Forest Baptist Health in Winston-Salem, North Carolina. His areas of special interest include sleep medicine, sleep apnea and critical care. He is also a member of the Public Safety Committee of the American Academy of Sleep Medicine.
Please visit the American Academy of Sleep Medicine to learn more.